New artificial cartilage mimics strength and suppleness of native cartilage
Composite material closest yet to properties of the real thing
December 17, 2013

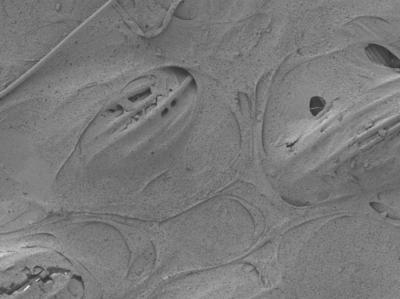
Tiny
interwoven fibers make up the three-dimensional fabric scaffold into
which a strong, pliable hydrogel is integrated and injected with stem
cells, forming a framework for growing cartilage. This image appears on
the cover of the Dec. 17, 2013, issue of Advanced Functional Materials.
(Credit: Frank Moutos, Farshid Guilak)
An article by lead authors Farshid Guilak, a professor of orthopedic surgery and biomedical engineering, and Xuanhe Zhao, assistant professor of mechanical engineering and materials science, appears today, Dec. 17 in the journal Advanced Functional Materials.
Articular cartilage is the tissue on the ends of bones where they meet at joints in the body — including in the knees, shoulders and hips. It can erode over time or be damaged by injury or overuse, causing pain and lack of mobility. While replacing the tissue could bring relief to millions, replicating the properties of native cartilage — which is strong and load-bearing, yet smooth and cushiony — has proven a challenge.
In 2007 Guilak and his team developed a three-dimensional fabric scaffold into which stem cells could be injected and successfully “grown” into articular cartilage tissue. Constructed of minuscule woven fibers, each of the scaffold’s seven layers is about as thick as a human hair. The finished product is about 1 millimeter thick.
Since then, the challenge has been to develop the right medium to fill the empty spaces of the scaffold — one that can sustain compressive loads, provide a lubricating surface and potentially support the growth of stem cells on the scaffold. Materials supple enough to simulate native cartilage have been too squishy and fragile to grow in a joint and withstand loading. “Think Jell-O,” says Guilak. Stronger substances, on the other hand, haven’t been smooth and flexible enough.
This
is a closer look at the scaffolding integrated with Xuanhe Zhao’s
hydrogel. The composite material, formed through a process comparable to
pouring concrete over a steel framework, may be a serviceable synthetic
replacement for the load-bearing cartilage found between bones.
(Credit: I-Chien Liao, Frank Moutos, Brad Estes
Zhao proposed a theory for the design of durable hydrogels (water-based polymer gels) and in 2012 collaborated with a team from Harvard University to develop an exceptionally strong yet pliable interpenetrating-network hydrogel.
“It’s extremely tough, flexible and formable, yet highly lubricating,” Zhao says. “It has all the mechanical properties of native cartilage and can withstand wear and tear without fracturing.”
He and Guilak began working together to integrate the hydrogel into the fabric of the 3-D woven scaffolds in a process Zhao compares to pouring concrete over a steel framework.
In their experiments, the researchers compared the resulting composite material to other combinations of Guilak’s scaffolding embedded with previously studied hydrogels. The tests showed that Zhao’s invention was tougher than the competition with a lower coefficient of friction. And though the resulting material did not quite meet the standards of natural cartilage, it easily outperformed all other known potential artificial replacements across the board, including the hydrogel and scaffolding by themselves.
“From a mechanical standpoint, this technology remedies the issues that other types of synthetic cartilage have had,” says Zhao, founder of Duke’s Soft Active Materials (SAMs) Laboratory. “It’s a very promising candidate for artificial cartilage in the future.”
The team’s next step will likely be to implant small patches of the synthetic cartilage in animal models, according to Guilak and Zhao.
“Once cartilage is damaged, it has little or no ability to repair itself,” Guilak explained to KurzweilAI. “This artificial cartilage has many of the properties of normal cartilage and could be used to repair damaged tissue. This approach is a significant advance over previous methods in that it combines a very tough “hydrogel”, which is soft and compliant, with a fiber reinforced matrix, which is strong and flexible. Thus this material has many similarities to normal cartilage, and thus should last much longer than standard materials.”
However, he said it will be “many years before this technology reaches the clinic. We are currently in the process of performing animal studies to determine how well it works. If successful, we will proceed to early human studies in 2–3 years.”
Their work was supported in part by the National Institutes of Health, the Arthritis Foundation, the Collaborative Research Center, AO Foundation, Davos, Switzerland and the NSF.
Abstract of Advanced Functional Materials paper
The development of synthetic biomaterials that possess mechanical properties mimicking those of native tissues remains an important challenge to the field of materials. In particular, articular cartilage is a complex nonlinear, viscoelastic, and anisotropic material that exhibits a very low coefficient of friction, allowing it to withstand millions of cycles of joint loading over decades of wear. Here, a three-dimensionally woven fiber scaffold that is infiltrated with an interpenetrating network hydrogel can build a functional biomaterial that provides the load-bearing and tribological properties of native cartilage. An interpenetrating dual-network “tough-gel” consisting of alginate and polyacrylamide was infused into a porous three-dimensionally woven poly(ϵ-caprolactone) fiber scaffold, providing a versatile fiber-reinforced composite structure as a potential acellular or cell-based replacement for cartilage repair.
(¯`*• Global Source and/or more resources at http://goo.gl/zvSV7 │ www.Future-Observatory.blogspot.com and on LinkeIn Group's "Becoming Aware of the Futures" at http://goo.gl/8qKBbK │ @SciCzar │ Point of Contact: www.linkedin.com/in/AndresAgostini
 Washington
Washington